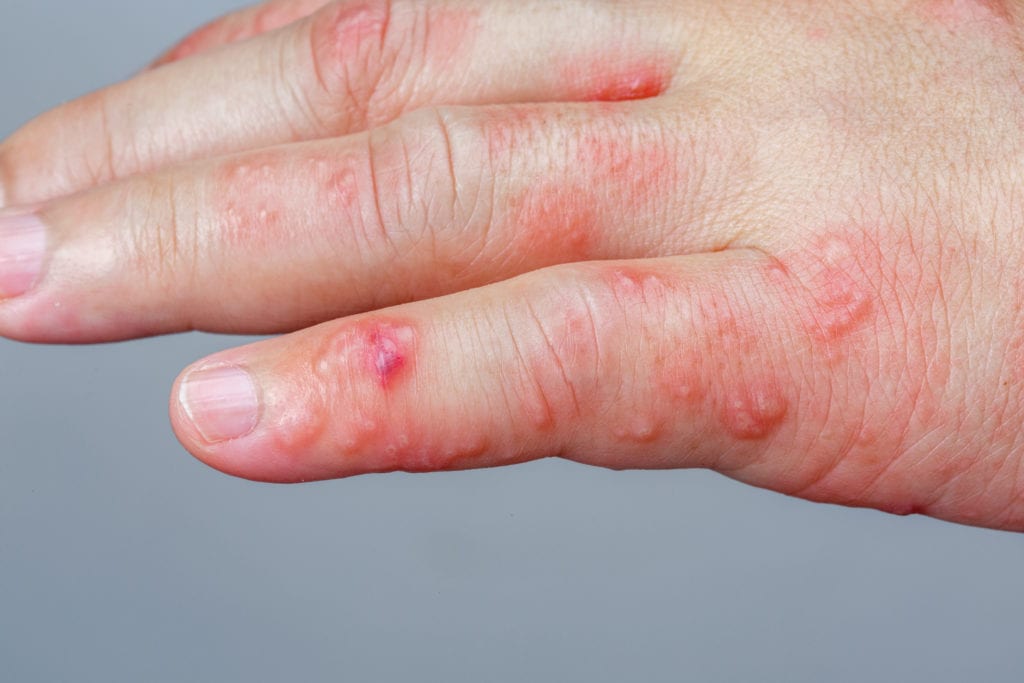
Of those, 1451 patients (mean age, 51.6 years 845 female) with a herpes zoster diagnosis were included in the primary SCRI analysis. Results Among 2 039 854 individuals who received any dose of a COVID-19 vaccine during the study period, the mean (SD) age was 43.2 (16.3) years 1 031 149 individuals (50.6%) were female, and 1 344 318 (65.9%) were White. Main Outcomes and Measures Incident herpes zoster, defined by International Statistical Classification of Diseases and Related Health Problems, Tenth Revision codes and a prescription of a new antiviral medication or a dose increase in antiviral medication within 5 days of diagnosis. Individuals included in the SCRI analysis were a subset of the COVID-19–vaccinated cohort who had herpes zoster during either a risk or control interval.Įxposures Any dose of a COVID-19 vaccine. A total of 2 039 854 individuals who received any dose of a COVID-19 vaccine with emergency use authorization (BNT162b2, mRNA-1273, or ) from December 11, 2020, through June 30, 2021, were eligible for inclusion. 
Data were obtained from Optum Labs Data Warehouse, a US national deidentified claims-based database. A supplemental cohort analysis was used to compare the risk of herpes zoster after COVID-19 vaccination with the risk of herpes zoster after influenza vaccination among 2 historical cohorts who received an influenza vaccine in the prepandemic period (January 1, 2018, to December 31, 2019) or the early pandemic period (March 1, 2020, to November 30, 2020). Objective To assess whether COVID-19 vaccination is associated with an increased risk of herpes zoster infection.ĭesign, Setting, and Participants This cohort study used a self-controlled risk interval (SCRI) design to compare the risk of herpes zoster in a risk interval of 30 days after COVID-19 vaccination or up to the date of the second vaccine dose with a control interval remote from COVID-19 vaccination (defined as 60-90 days after the last recorded vaccination date for each individual, allowing for a 30-day washout period between control and risk intervals). It is not known whether these cases represent increased reporting or a true increase in risk. Importance Herpes zoster infection after COVID-19 vaccination has been reported in numerous case studies. Shared Decision Making and Communication.Scientific Discovery and the Future of Medicine.Health Care Economics, Insurance, Payment.Clinical Implications of Basic Neuroscience.Challenges in Clinical Electrocardiography.Comparison of Adjusted Hazard Ratios of Vaccination Type (COVID-19 vs Prepandemic Influenza and COVID-19 vs Early Pandemic Influenza) for Herpes Zoster and 3 Negative Control Outcomes Risk of Herpes Zoster Infection Among COVID-19 Vaccinated vs Influenza Vaccinated, Early PandemicĮTable 13. Risk of Herpes Zoster Infection Among COVID-19 Vaccinated vs Influenza Vaccinated, PrepandemicĮTable 12. Characteristics of Cohort Study Population by Vaccine ExposureĮTable 11. Negative Control Outcomes and Corresponding ICD-10 CodesĮTable 10. Systemic Corticosteroids and Other Immunosuppressants Used to Determine Covariate StatusĮTable 8. ICD-10 Codes and Descriptions Used to Identify COVID-19 InfectionĮTable 9. Search Terms Used to Identify Herpes Zoster Vaccination StatusĮTable 7. 
Procedure Codes for Influenza Vaccines From January 1, 2018, Through July 31, 2021ĮTable 5. ICD-10 Codes Used to Identify Comorbidity StatusĮTable 6. Antiviral Medications and Dose Levels Used to Identify Herpes Zoster Outcome and Covariate StatusĮTable 4. Corticosteroids Used to Identify Herpes Zoster OutcomeĮTable 3. Procedure and Drug Codes for COVID-19 Vaccines From December 11, 2020, Through June 30, 2021ĮTable 2. Study Design and Population Flow DiagramĮTable 1.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
